All You Need to Know About Ventilators
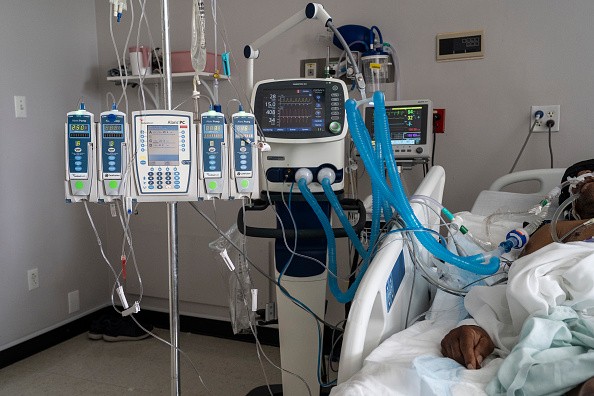
(Photo : Go Nakamura / Stringer)
In simple terms, ventilators help the lungs of a patient who cannot breathe independently breathe. It is also known as a respirator or a breathing machine, or mechanical ventilation. A ventilator is computerized and controlled by microprocessors, and it is used in intensive care medicine, emergency medicine, home care, and anesthesia. It is not only used to help a patient with breathing difficulty or respiratory disease but also during a surgical operation. Especially after anesthesia has been administered and after surgery to help the recovering patient breathe for long hours or days.
Some of the medical conditions that require ventilators include polio, pneumonia, stroke, coma, upper spinal cord injury, premature lung development in babies, and in recent times, coronavirus (COVID-19).
A ventilator gets oxygen into the human body and removes carbon dioxide from it. It is installed by a process called intubation, which involves the insertion of a tube into the mouth or lungs of the patient. Some cases require tracheostomy which is a surgery done to make a small hole in the patient's neck. Ventilators generally run-on electricity but some types are powered by batteries.
Some expectations that come with being a patient on a ventilator include:
-
Discomfort due to inability to talk or move around even when conscious.
-
Medications such as pain relievers, sedatives, muscle relaxers, sleep medication generally cause drowsiness and confusion. The effects fade off when the dosage stops and are no more needed as soon as the patient stops using the ventilator.
-
Monitoring of the health conditions especially heart rate, blood pressure, breathing, chest X-ray, and oxygen saturation as well as blood tests to check the amount of oxygenated and deoxygenated blood.
The coronavirus pandemic has made the use of ventilators widespread and popular. If a patient of coronavirus is not able to fight off the infection by the immune system, it leads to Acute Respiratory Distress Syndrome (ARDS) in which the air sacs which are meant to help make the blood oxygenated become filled with fluid and stops the lungs from supplying vital organs with oxygen. A patient in this condition is in a life-threatening situation and certainly needs to be on a ventilator.
The use of ventilators is indeed lifesaving and necessary for life-threatening respiratory conditions. Several people who have survived COVID-19 cases could not have made it without ventilators. However, they also come with some side effects and potential risks that occur with prolonged use. Some of these risks include:
-
Infection of airborne diseases: ventilators cannot protect against airborne infections like Sinus infections and pneumonia. Antibiotics are usually included in the patient's medications to protect against such infections. The ventilator can also cause blood clots and skin infections.
-
Discomfort and irritation due to the breathing tube rubbing against the throat or lungs. Coughing will also be difficult, as coughing is the body's mechanism for removing dust, food particles, water, smoke, and other irritants from the lungs. The ventilator's breathing tube can also damage the voice box and cause difficulty in speaking or breathing.
-
Damage to the lungs: injury to the lungs can occur because of too much pressure in the lungs, causing oxygen toxicity. Oxygen toxicity is too much oxygen in the lungs and air leaking into the space between the chest wall and lungs. However, with a guide on the use of oxygen sensors, be monitored.
-
Cognitive and mental issues: such as delirium and Post-Traumatic Disorder (PTSD), often occur after the patients have unplugged from the ventilators.
See Now: NASA's Juno Spacecraft's Rendezvous With Jupiter's Mammoth Cyclone
* This is a contributed article and this content does not necessarily represent the views of scienceworldreport.com



Join the Conversation